
La Dra. Sandra Gracia López posee sobre 25 años de experiencia en el campo de Medicina Nuclear, y un prominente récord de logros y reconocimientos en los sectores públicos y privados incluyendo la Escuela de Medicina de la Universidad de Puerto Rico y más reciente aún, las tres facilidades del Hospital de Menonita en Puerto Rico. A continuación se ofrece un breve resumen de experiencia, educación, logros y certificaciones, en el campo de Medicina Nuclear, alcanzados por la doctora Gracia:
Obtuvo su título como Doctora en Medicina en el 1981, en la Escuela de Medicina de Ponce. Posteriormente, completó su residencia en Medicina Interna en el Hospital Damas de Ponce, trabajó durante dos años como especialista en Medicina Interna y posteriormente terminó su fellowship en Medicina Nuclear en el Recinto de Ciencias Médicas de la Escuela de Medicina de Puerto Rico. Durante su segundo año en Medicina Nuclear obtuvo una pasantía de varios meses en el Departamento de Medicina.
We are an integrated team of professionals in the field, certified by the American Board of Nuclear Medicine Technology, the American Board of Nuclear Medicine and the American Board of Nuclear Cardiology who have been working in the specialty field for a long time. Some of us have 27 years of experience in Internal Medicine and Nuclear Medicine/Live Molecular Imaging and are Board certified in Nuclear Medicine and Nuclear Cardiology. Our team also includes Cardiologists, a Physicist and Administrative Personnel with excellent skills in customer service. Furthermore, we have expertise in radiation protection and have a wealth of training and experience in developing exercises and in the organization of drills related to radiation incidents and accidents and how to manage their consequences.
Our team has achieved certifications by Joint Commission and the Intersocietal Accreditation Council in Nuclear Medicine, Nuclear Cardiology and PET-CT. Recognized by local and international patients for the excellent customer service we provide, it is our goal to help our patients and referring physicians enjoy their experience and make better informed diagnostic and treatment decisions.

Sección de Videos
Molecular Imaging is the next step in personalized medicine. We can see pathology early while in its initial stages when it is possible to prevent progression of diseases such as myocardial or cerebral ischemia. We can see malignant tumors early in their development to be able to excise them surgically and we can see what chemotherapy is doing to eliminate tumoral mass and to cure the patients. With molecular imaging we can alert treating physicians when therapy is not being effective and when other options may be curative for their patients. Actually, it is possible to find pathology long before there are symptoms in diseases such as Alzheimer’s dementia and we can also use the information to select the best therapy for a specific patient. All this can be done because we are evaluating physiological changes at the molecular level, when we can improve the future quality of the life of our patients.

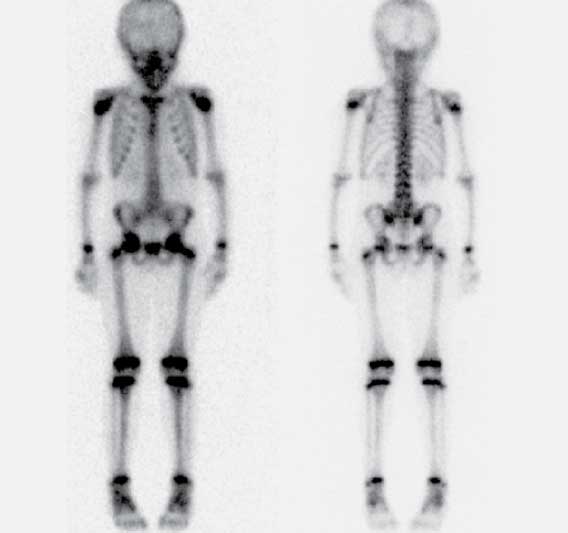
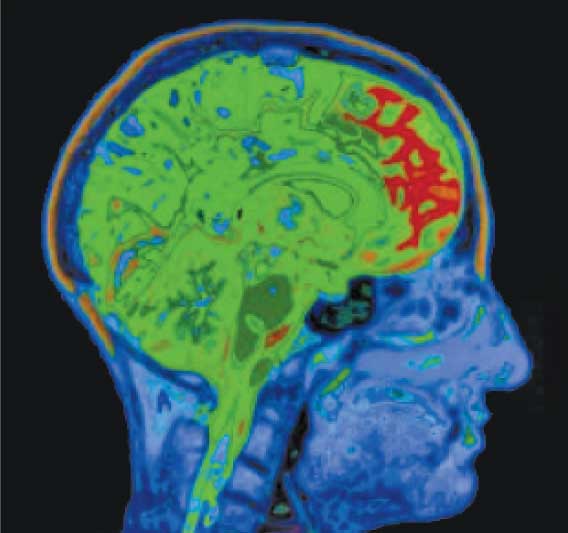
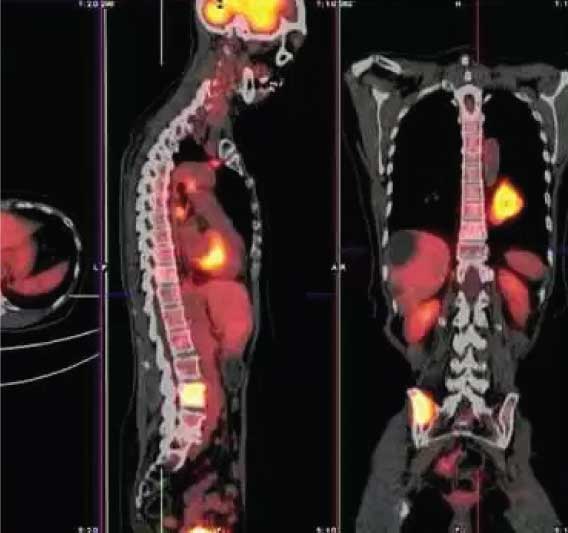
Molecular images are detailed pictures of what is happening inside the organs of live bodies. The images created are really a picture of what is happening in the
cells and the molecules that make up those cells. The techniques that see structure and size allow us to see the organs but do not necessarily indicate their
function. For example, we can have a normal size heart or gallbladder, in its expected location and with a normal shape but that does not necessarily mean that
the organ has normal function. It is common to see a normal structure (anatomy) but abnormal function (physiology). Usually, the change in the function occurs
earlier than the change in the size of the organs and because of that, we can make earlier diagnoses, at times when many diseases or conditions can be cured.
One of the most common examples is the coronary artery disease: when the obstruction of the artery affects the delivery of the blood to the cardiac muscle, we
can change our habits (dietary, exercise and medications) that may cause the plaques that obstruct those arteries to stop growing. Sometimes, when
obstructions are severe, the only alternative is coronary surgery and in those cases, with Molecular Imaging we can evaluate which area of the heart is most
affected and whether surgery will prevent permanent cardiac muscle damage.
What has been known during decades, as Nuclear Medicine is really Molecular Imaging. This is so because the amount of radiopharmaceuticals that is
administered is minimal and it goes to the cells we need to see and study. These techniques allow the physician to see how the organ or organ system works and
also to measure the biological processes, for example, the function of the heart muscle and the contraction or the gallbladder. In addition, we can detect
problems with the function of the organs and systems before the patient has symptoms. This happens frequently in cancer, when we see very small tumors and
the patient has no symptoms, either before or after treatment.
Molecular Medicine allows us access to the bodily functions to personalize the treatment of the patients. This because we can see the severity of the disease, the
extension of a large amount of tumors, the response of the patient to diferent therapies and the progression of the diseases. Sometimes we can measure the
response of the organ after a specific treatment such as the improvement in the function of kidneys that were obstructed, after the removal of kidney stones,
improvement in the cardiac function after diferent types of surgeries, the improvement in the function of the liver after the patient stops the ingestion of
exaggerated amounts of alcoholic beverages and may.
A team of experienced experts in the field.
If we can see abnormalities in the function of our organs and systems while we are still strong and can undergo treatments with medications or surgeries, the outcomes of those treatments may be better and we may be able to remain healthier for a longer time. In addition, as all the information is integrated regarding blood changes, organ function changes and symptoms, we may be able to decide in collaboration with the patients and a variety of specialist, what the best treatment is for them and even integrate alternative methods such as acupuncture and others, in the therapeutic plans. In certain cases, if we cannot attempt cure, we may be able to provide palliative treatments to maintain a good quality of life instead of providing aggressive therapy if the disease is at a too advanced stage.
Más información

